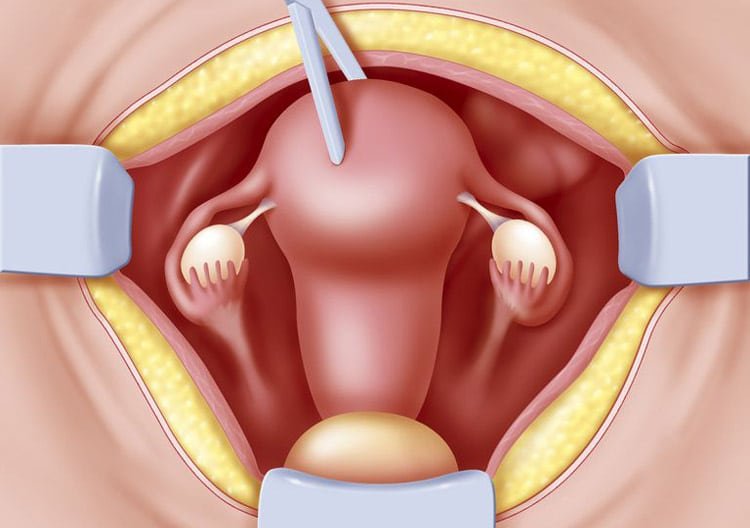
What Is a Hysterectomy?
At Sparsh Hospital, hysterectomies are performed using advanced minimally invasive techniques to ensure:
Less pain
Smaller incisions
Minimal blood loss
Faster healing
Short hospital stay
Who Needs a Hysterectomy?
Doctors recommend a hysterectomy only when other medical treatments or medications do not control the condition. It is mainly suggested for:
1. Uterine Fibroids
Non-cancerous growths that cause heavy bleeding, pain, or pressure.
2. Adenomyosis
When the inner lining of the uterus grows into the muscle wall, leading to severe cramps and heavy periods.
3. Endometriosis
Tissue similar to the uterine lining grows outside the uterus, causing chronic pelvic pain.
4. Severe Abnormal Uterine Bleeding
Prolonged or heavy bleeding unresponsive to medicines or other procedures.
5. Uterine Prolapse
When the uterus drops from its normal position due to weak pelvic muscles, causing discomfort and urinary issues.
6. Chronic Pelvic Pain
Long-term pain that affects daily life and is not treatable through medicines.
7. Cancer
A hysterectomy may be required in cases of:
Uterine cancer
Cervical cancer
Ovarian cancer
Endometrial cancer
Types of Hysterectomy at Sparsh Hospital
At Sparsh Hospital, your surgeon recommends the most suitable type based on your condition, age, fertility goals, and overall health.
1. Total Hysterectomy
Removal of the uterus and cervix.
Most commonly performed procedure.
2. Partial (Subtotal) Hysterectomy
Only the upper part of the uterus is removed.
The cervix is left intact.
3. Radical Hysterectomy
Used mainly for cancer cases. Includes removal of uterus, cervix, top part of vagina, and surrounding tissues.
4. Hysterectomy With Salpingo-Oophorectomy
Removal of:
Uterus
Fallopian tubes
Ovaries
This is often recommended for severe diseases or cancer.
Surgical Techniques Available at Sparsh Hospital
1. Laparoscopic Hysterectomy (Minimal Invasive)
This is the most preferred technique at Sparsh Hospital.
Benefits:
✔ Small incisions
✔ Less pain
✔ Very less blood loss
✔ Faster recovery
✔ Shorter hospital stay
✔ Minimal scarring
2. Vaginal Hysterectomy
The uterus is removed through the vagina without any abdominal cut.
Benefits:
✔ No visible scar
✔ Quick healing
✔ Shorter recovery time
3. Abdominal Hysterectomy
Performed through a larger incision in the lower abdomen.
Recommended only for large fibroids, complex diseases, or cancer.
4. LAVH (Laparoscopic-Assisted Vaginal Hysterectomy)
Combination of laparoscopy and vaginal removal for precise and safe results.
How to Prepare for a Hysterectomy?
Before the surgery, your doctor at Sparsh Hospital will perform a detailed evaluation.
Pre-surgical Assessment Includes:
Pelvic ultrasound
Blood tests
ECG
Pap smear
MRI/CT (if needed)
Review of medical history
Pregnancy test (for women of reproductive age)
Pre-surgery Instructions:
Avoid eating and drinking 6–8 hours before surgery
Stop certain medications (your doctor will guide you)
Arrange someone to accompany you
Follow hygiene and pre-surgical bathing instructions
Step-by-Step Procedure of Hysterectomy
1. Anesthesia
General or spinal anesthesia ensures you feel no pain during surgery.
2. Incisions
Depending on the method, small or larger incisions are made.
3. Removal of the Uterus
The surgeon carefully separates the uterus from surrounding structures.
4. Closure
Incisions are closed with sutures or surgical glue.
Duration:
Most procedures take 1–2 hours.
Benefits of Hysterectomy
1. Relief From Pain
Eliminates chronic pelvic pain, cramps, and discomfort.
2. Stops Heavy Bleeding
No more excessive periods or bleeding-related anemia.
3. Better Quality of Life
Improved mobility, comfort, sleep, and daily functioning.
4. Treatment for Cancer
Prevents spread and improves survival chances.
5. Eliminates Risk of Uterine Diseases
No future risk of fibroids, adenomyosis, or uterine infections.
Recovery After Hysterectomy
Recovery depends on the type of surgery, but patients at Sparsh Hospital typically heal faster due to minimally invasive techniques.
Hospital Stay:
Laparoscopic/Vaginal: 24–48 hours
Abdominal: 2–4 days
Recovery Timeline:
Return to light work: 2–3 weeks
Full recovery: 4–6 weeks
Post-Surgery Guidelines:
Avoid heavy lifting for 6 weeks
Take prescribed medications
Keep the incision area clean
Start walking early to prevent blood clots
Avoid intercourse for 6–8 weeks
Follow-up visits at scheduled times
Life After Hysterectomy
Periods Stop Completely
No menstrual bleeding after surgery.
Hormonal Changes
If ovaries are removed, you may experience menopause. Doctors may prescribe hormone therapy if needed.
Sexual Life
Most women resume normal sexual activity after complete healing.
Emotional Well-being
Some women feel emotional changes; counseling and support are available at Sparsh Hospital.
