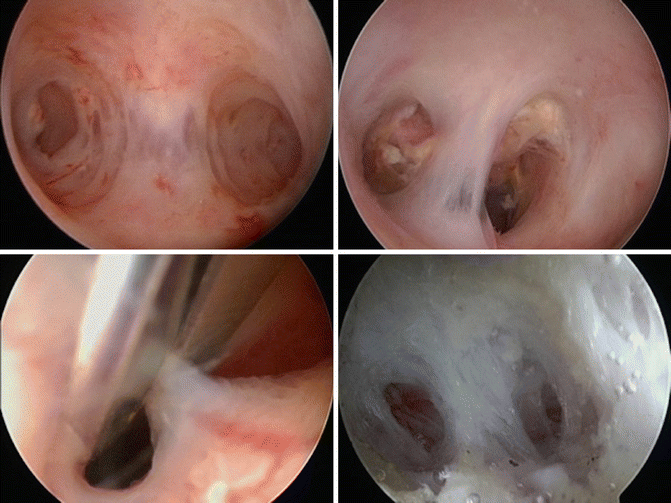
What Is Hysteroscopy?
Hysteroscopy is a minimally invasive gynecological procedure in which a thin, lighted instrument called a hysteroscope is gently passed through the vagina and cervix into the uterus. This allows the doctor to examine the uterine cavity in real time.
There are two main types:
Diagnostic Hysteroscopy – Used to identify uterine problems
Operative Hysteroscopy – Used to treat detected abnormalities in the same sitting
At Sparsh Hospital, we often combine diagnosis and treatment in a single procedure, thereby reducing hospital visits, cost, and recovery time.
Conditions Treated with Hysteroscopy at Sparsh Hospital
1. Hysteroscopy for Uterine Septum
A uterine septum is a congenital condition where a fibrous or muscular wall divides the uterine cavity partially or completely. Although many women are asymptomatic, a uterine septum is strongly associated with:
Recurrent miscarriages
Infertility
Preterm labor
Implantation failure during IVF
How Hysteroscopy Helps
Hysteroscopic septal resection is a safe and effective treatment. Using fine instruments, the septum is carefully removed under direct visualization, restoring the normal uterine shape.
Benefits
Improves fertility outcomes
Reduces miscarriage risk
No external cuts or scars
Preserves the uterus
At Sparsh Hospital, this procedure is performed by skilled gynecologists with expertise in fertility-preserving surgeries.
2. Hysteroscopy for Endometrial Polyps
Endometrial polyps are soft tissue growths arising from the uterine lining. While usually benign, they can cause significant symptoms such as:
Heavy or irregular menstrual bleeding
Spotting between periods
Infertility
Failed embryo implantation
Hysteroscopic Polypectomy
Hysteroscopy is the most accurate method to diagnose and remove uterine polyps. During the procedure, the polyp is visualized and removed completely from its base, reducing the risk of recurrence.
Why Removal Is Important
Improves chances of natural conception and IVF success
Stops abnormal bleeding
Prevents potential malignant changes
At Sparsh Hospital, removed polyps are sent for histopathological examination to ensure patient safety and peace of mind.
3. Hysteroscopy for Intrauterine Adhesions (Asherman’s Syndrome)
Intrauterine adhesions occur when scar tissue forms inside the uterus, often after:
Dilation and curettage (D&C)
Previous uterine surgery
Infections such as tuberculosis or endometritis
These adhesions may lead to:
Absent or scanty periods
Infertility
Recurrent pregnancy loss
Pelvic pain
Hysteroscopic Adhesiolysis
Hysteroscopy is the only definitive method to diagnose and treat intrauterine adhesions. Scar tissue is gently cut and removed, restoring the uterine cavity.
Post-Procedure Care
To prevent recurrence, patients may receive:
Hormonal therapy
Intrauterine balloon or gel
Follow-up hysteroscopy
At Sparsh Hospital, we follow international protocols to ensure optimal healing and long-term results.
Who Needs Hysteroscopy?
Hysteroscopy is recommended for women experiencing:
Infertility or repeated IVF failure
Recurrent miscarriages
Heavy, irregular, or painful periods
Abnormal ultrasound findings
Suspected uterine abnormalities
Post-menopausal bleeding
Our specialists at Sparsh Hospital conduct thorough evaluations before recommending hysteroscopy, ensuring it is truly beneficial for the patient.
How Is Hysteroscopy Performed?
Before the Procedure
Detailed consultation and ultrasound
Blood tests if required
Procedure scheduled in early menstrual phase
Short fasting if anesthesia is planned
During the Procedure
Performed under local, spinal, or short general anesthesia
Hysteroscope inserted gently through the cervix
Uterine cavity expanded using saline
Abnormalities visualized and treated
Duration
Diagnostic: 10–15 minutes
Operative: 30–45 minutes
After the Procedure
Same-day discharge in most cases
Mild cramps or spotting for 1–2 days
Return to normal activity within 24–48 hours
Advantages of Hysteroscopy at Sparsh Hospital
✔ Experienced gynecologists & fertility specialists
✔ Advanced hysteroscopy equipment
✔ Minimally invasive, uterus-saving procedures
✔ Day-care surgery with quick recovery
✔ High success rates in infertility management
✔ Personalized patient care and counseling
We focus not only on treatment but also on patient education and emotional support, especially for women dealing with infertility or pregnancy loss.
Hysteroscopy and Infertility Treatment
Hysteroscopy plays a vital role in fertility care, particularly before IVF or IUI. Correcting uterine abnormalities significantly improves implantation rates and pregnancy outcomes.
At Sparsh Hospital, hysteroscopy is often integrated with:
Basic fertility evaluation
Ovulation induction
IUI
IVF & advanced reproductive techniques
This comprehensive approach ensures better results and patient satisfaction.
Is Hysteroscopy Safe?
Yes, hysteroscopy is a very safe procedure when performed by trained specialists. However, like all medical procedures, minimal risks may include:
Infection
Uterine perforation (rare)
Mild bleeding
At Sparsh Hospital, strict safety protocols and sterile techniques are followed to minimize risks.
Recovery and Results
Most women:
Resume normal activities within 1–2 days
Experience improved menstrual cycles
Show better fertility outcomes
Have reduced pain and bleeding
Follow-up visits are scheduled to monitor healing and plan further treatment if needed.
