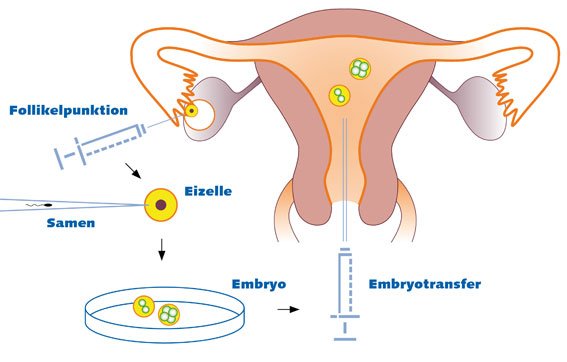
What is ICSI?
Intracytoplasmic Sperm Injection (ICSI) is a specialized form of In Vitro Fertilization (IVF) used to treat severe male factor infertility and other fertilization challenges. In traditional IVF, many healthy sperm are placed near an egg to allow natural fertilization. However, in ICSI, a single healthy sperm is carefully selected and injected directly into the cytoplasm of the egg using a microscopic needle.
Key Advantages of ICSI:
High success in cases of male factor infertility
Effective for low sperm count or poor sperm motility
Can be used with previously frozen eggs or sperm
Facilitates fertilization in cases where IVF has failed
Enables genetic testing and embryo selection
Who Needs ICSI? – Indications
ICSI is recommended when one or more of the following conditions exist:
Male Factor Infertility
Low sperm count (oligospermia)
No sperm in ejaculate (azoospermia) — sperm obtained by surgical retrieval
Poor sperm motility or morphology
Previous IVF cycles with failed fertilization
Female or Unexplained Fertility Issues
Advanced maternal age
Thick zona pellucida (outer shell of egg)
Prior IVF cycles with poor fertilization
Use of frozen eggs
Other Reasons
Genetic testing (PGT) requirements
Use of donor eggs or sperm
Couples with repeated implantation failure
At Sparsh Hospital, every couple undergoes detailed fertility evaluation to determine if ICSI is the most suitable option.
Step-by-Step: The ICSI Process
1. Initial Consultation & Evaluation
Your fertility journey begins with a comprehensive consultation with our reproductive specialists. We assess medical history, perform physical examinations, and recommend appropriate hormonal and diagnostic tests for both partners.
Evaluations include:
Semen analysis
Hormonal profiling
Ultrasound of female reproductive organs
Infectious disease screening
2. Ovarian Stimulation
The female partner receives tailored hormonal medications to stimulate the development of multiple eggs. Throughout this phase, we monitor follicle growth with regular ultrasounds and hormone tests to ensure optimal timing for egg retrieval.
3. Sperm Preparation
On the day of egg retrieval, a semen sample is collected and prepared in our state-of-the-art embryology lab. If needed, sperm can also be retrieved via surgical procedures such as:
TESA (Testicular Sperm Aspiration)
PESA (Percutaneous Epididymal Sperm Aspiration)
Our embryologists assess and select the most suitable sperm for injection.
4. Egg Retrieval
Performed under mild sedation, this minimally invasive procedure involves retrieving mature eggs from the ovaries using an ultrasound-guided needle. Patients typically return home the same day.
5. The ICSI Procedure
In the embryology lab:
Each mature egg is held gently with a microscopic pipette.
A single sperm is immobilized and injected directly into the egg’s cytoplasm using precision micromanipulation tools.
Injected eggs are then placed in a controlled culture environment for embryo development.
6. Fertilization Check & Embryo Culture
Approximately 16-18 hours after injection, embryologists assess fertilization. Fertilized eggs (zygotes) are cultured and monitored closely to track their development into embryos.
7. Embryo Transfer
After 3–5 days of culture, one or more healthy embryos are selected and transferred into the uterus using a thin catheter. This gentle procedure is typically painless and done without anesthesia.
8. Luteal Support & Pregnancy Test
Post-transfer, hormone support (progesterone) helps prepare the uterine lining for implantation. A pregnancy blood test is scheduled approximately 10–14 days after embryo transfer.
Success Rates and What to Expect
Success depends on several factors:
Age of the female partner
Cause of infertility
Egg and sperm quality
Embryo health
Previous fertility treatments
At Sparsh Hospital, our success rates are comparable with leading fertility centers internationally. We provide transparent counseling on realistic expectations and personalized timelines.
Advantages of ICSI at Sparsh Hospital
World-Class Embryology Lab
Our fully equipped laboratory uses the latest micromanipulation technology and culture systems to support optimal fertilization and embryo growth.
Experienced Fertility Team
Our team includes:
Fertility specialists with extensive clinical experience
Certified embryologists trained in advanced micromanipulation techniques
Support staff dedicated to patient care and emotional support
Personalized Treatment Plans
No two fertility journeys are the same. We design every ICSI cycle based on individual health, diagnostics, history, and preferences.
Safety and Ethical Standards
We adhere to strict safety protocols, ethical guidelines, and patient confidentiality policies. Your safety and dignity are our priority.
Emotional and Psychological Support
Infertility treatment can be emotionally challenging. We provide counseling services and support groups to help you stay strong throughout your journey.
Financial Guidance and Support
We offer transparent pricing and help you understand costs involved. Our financial counselors can assist with planning and insurance queries where applicable.
Frequently Asked Questions
1. Is ICSI painful?
ICSI itself is not painful. Egg retrieval is done under sedation, and embryo transfer is usually painless. Some women may experience mild cramping or spotting afterward.
2. How many embryos should be transferred?
The number depends on age, embryo quality, and medical history. We follow guidelines to minimize the risk of multiple pregnancies while maximizing success.
3. Are there any risks?
Like any medical procedure, ICSI carries minor risks such as ovarian hyperstimulation or multiple pregnancy. Serious complications are rare, and we take preventative measures.
4. What happens to unused embryos?
You have options:
Cryopreservation (freezing for future use)
Donation
Disposal according to your preferences and ethical guidelines
5. Can ICSI be done with donor sperm or eggs?
Yes. ICSI can be performed using donor gametes based on your treatment plan.
