What are IMSI and PICSI?
IMSI — High-magnification morphologic sperm selection
IMSI uses a high-magnification microscope (typically ×6,000 to ×10,000) to examine individual sperm in much finer detail than standard ICSI (which uses ×400 magnification). This allows embryologists to identify subtle abnormalities in the sperm head, acrosome or nuclear content — features that are linked to DNA damage and poor embryo outcomes — and to select sperm that appear morphologically optimal for injection into the oocyte.
PICSI — Physiologic selection using hyaluronic acid binding
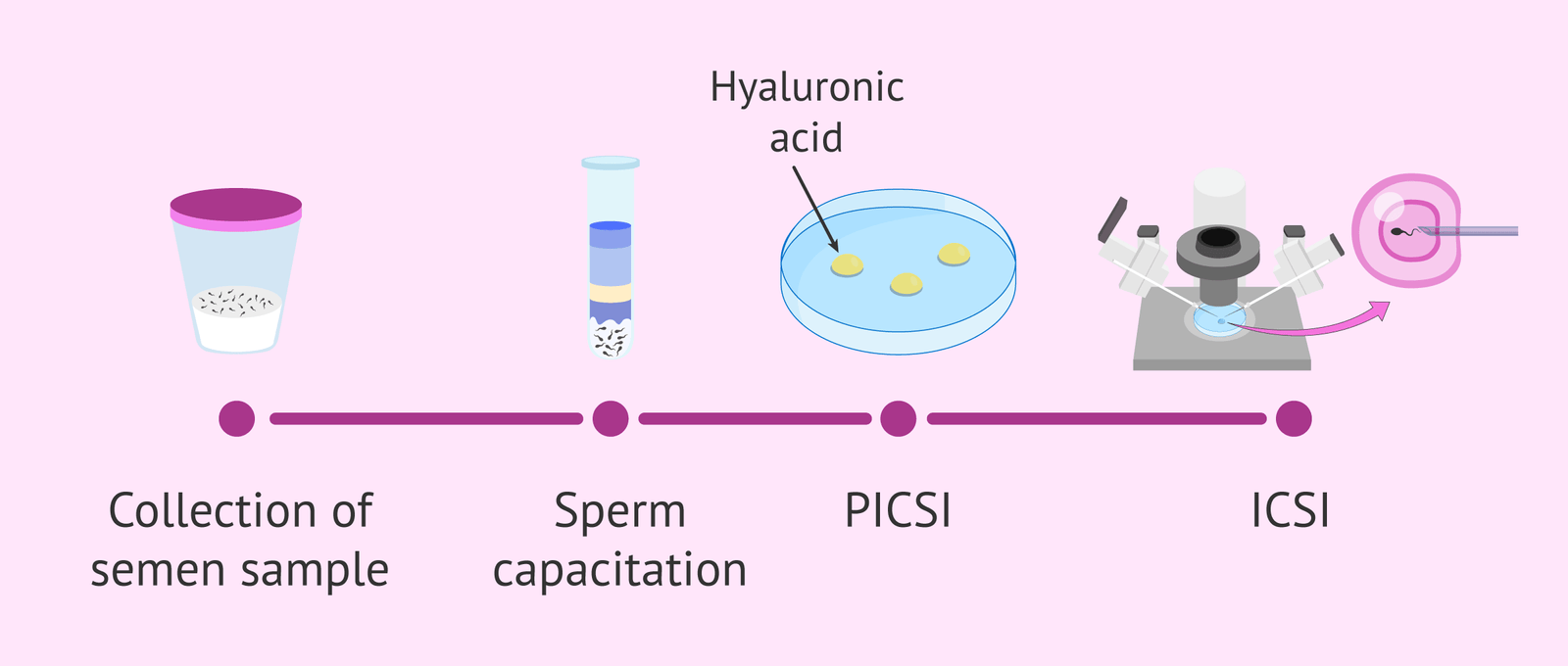
PICSI relies on the natural affinity of mature, functionally competent sperm to bind to hyaluronic acid (HA). In a PICSI dish, sperm that bind to HA are considered more mature and have lower rates of DNA fragmentation. The embryologist selects HA-bound sperm for ICSI, combining physiologic selection with standard ICSI injection techniques.
Who is a candidate for IMSI or PICSI?
IMSI or PICSI may be recommended for:
Couples with male-factor infertility (severe teratozoospermia, poor morphology, oligozoospermia, or asthenozoospermia).
Couples with repeated IVF/ICSI failures despite good embryo transfer technique.
Men with high sperm DNA fragmentation or abnormal sperm chromatin structure.
Couples seeking to maximize embryo quality when egg numbers are limited.
Cases of advanced paternal age where subtle sperm defects may be more prevalent.
Couples wanting every available advantage in select complex infertility scenarios.
Your fertility specialist at Sparsh will evaluate semen analysis, past IVF history, age, and diagnostic tests (including DNA fragmentation testing if available) to recommend the most appropriate approach.
How IMSI and PICSI are performed — step by step
Both procedures are integrated into the standard IVF/ICSI laboratory workflow. Below is a concise outline of each technique within an IVF cycle.
Common preparatory steps (IVF cycle basics)
Ovarian stimulation & egg retrieval: The female partner undergoes controlled ovarian stimulation followed by transvaginal ultrasound-guided oocyte retrieval.
Semen collection & processing: Male partner provides a semen sample on the day of retrieval, which is processed to isolate motile sperm.
IMSI procedure
Processed sperm are placed under a specialized high-magnification inverted microscope.
Embryologist inspects many individual sperm at ×6,000–10,000 magnification to evaluate head shape, vacuoles, acrosomal status and nuclear appearance.
Sperm with the best morphological profile (minimal vacuoles, normal head shape, intact acrosome) are selected.
Selected sperm are immobilized and injected into the mature oocytes using standard microinjection technique (ICSI).
Fertilization is assessed 16–18 hours later and embryo development is monitored.
PICSI procedure
Sperm are placed on a PICSI dish containing hyaluronic-acid treated microdots.
Motile sperm that bind to HA droplets are identified and considered physiologically mature.
HA-bound sperm are retrieved with a micropipette, immobilized, and used for microinjection into oocytes (ICSI).
Embryos are monitored as in a standard IVF cycle.
Benefits — why choose IMSI or PICSI?
While no technique guarantees pregnancy, IMSI and PICSI offer several potential advantages in appropriately selected cases:
Improved sperm selection: Both methods aim to select sperm with fewer structural defects or better functional maturity.
Potentially higher fertilization quality: Selecting higher-quality sperm may lead to improved fertilization and embryo development.
Better embryo morphology: Some studies and clinical experience report improved embryo grading with advanced sperm selection.
Reduced rates of genetic and chromosomal abnormalities (potentially): By avoiding sperm with severe nuclear defects, these methods aim to lower the likelihood of transmitting damaged DNA.
Useful after repeated IVF failures: IMSI and PICSI are valuable options when standard ICSI has not produced a viable pregnancy.
Minimally invasive to the female partner: The additional laboratory steps do not alter the ovarian stimulation or retrieval process.
At Sparsh Hospital our experienced embryology team carefully selects the appropriate method — IMSI, PICSI, or conventional ICSI — tailored to each couple’s diagnostic profile.
Risks and limitations
No absolute guarantee: While IMSI/PICSI can improve selection, they cannot guarantee pregnancy or eliminate all risks related to embryos or genetic abnormalities.
Cost and availability: These are specialized laboratory procedures and may add cost to the IVF cycle. Sparsh Hospital will provide clear pricing and counseling.
Time and laboratory resources: IMSI requires more microscope time and operator skill; PICSI requires specific consumables. Both require trained embryologists.
Not always necessary: For couples with normal semen parameters and no history of IVF failure, standard ICSI or conventional IVF may be sufficient.
Your fertility specialist will discuss whether the potential benefits outweigh limitations in your specific case.
Success factors — what influences outcomes?
Several variables affect how well IMSI or PICSI may perform for an individual couple:
Female age and egg quality: Egg quality is a major determinant of embryo health; better eggs increase success regardless of sperm selection.
Number of retrieved oocytes: More oocytes provide more opportunities to create high-quality embryos.
Underlying sperm issues: The degree and type of sperm abnormality influence outcomes; in severe cases, surgical sperm retrieval or donor sperm may be discussed.
Laboratory expertise: The skill of the embryology team and the quality of the IVF lab are critical. Sparsh Hospital emphasizes rigorous quality control and experienced embryologists.
Overall reproductive health: Uterine and endometrial factors, immunologic issues, and female reproductive conditions also matter.
Sparsh’s multidisciplinary team assesses these factors to build a personalized treatment plan.
Frequently Asked Questions (FAQs)
Q: Which is better — IMSI or PICSI?
A: They are different approaches. IMSI is morphological (very high magnification), while PICSI is functional (HA-binding). Choice depends on semen findings, prior IVF history and diagnostic tests. Your doctor will recommend the most suitable option.
Q: Does IMSI/PICSI increase congenital anomalies?
A: There is no conclusive evidence that IMSI or PICSI increases congenital anomalies when performed by experienced teams. These techniques aim to select healthier sperm. Genetic counseling may be offered when indicated.
Q: How much extra time does IMSI add?
A: IMSI is more time-intensive in the lab because embryologists inspect sperm at very high magnification. This does not change ovarian stimulation or egg retrieval timing.
Q: Is PICSI painful or invasive?
A: No — PICSI is a laboratory procedure applied to the sperm sample only. It does not add invasive steps for the female partner beyond standard IVF/ICSI.
Q: Should men get DNA fragmentation testing before IMSI/PICSI?
A: DNA fragmentation testing can be helpful to evaluate why IVF/ICSI may have failed previously. It may influence the decision to use PICSI, IMSI, antioxidant therapy, or surgical sperm retrieval.
Why choose Sparsh Hospital for IMSI & PICSI?
Experienced embryology team: Our embryologists are trained in advanced sperm selection methods and microinjection techniques.
State-of-the-art laboratory: ISO-level quality systems, advanced microscopes, controlled environments and strict quality control ensure precise handling.
Individualized care: Treatment recommendations at Sparsh are based on diagnostic testing, previous cycle history, and couples’ goals.
Comprehensive fertility services: From preconception counseling and diagnostic testing to IVF, genetic testing and pregnancy support, we provide end-to-end fertility care.
Transparent counseling & pricing: We provide clear explanations, expected outcomes and costs so couples can make informed decisions.
Supportive environment: Emotional counseling and patient education are integrated into care; infertility treatment is a team effort at Sparsh.
