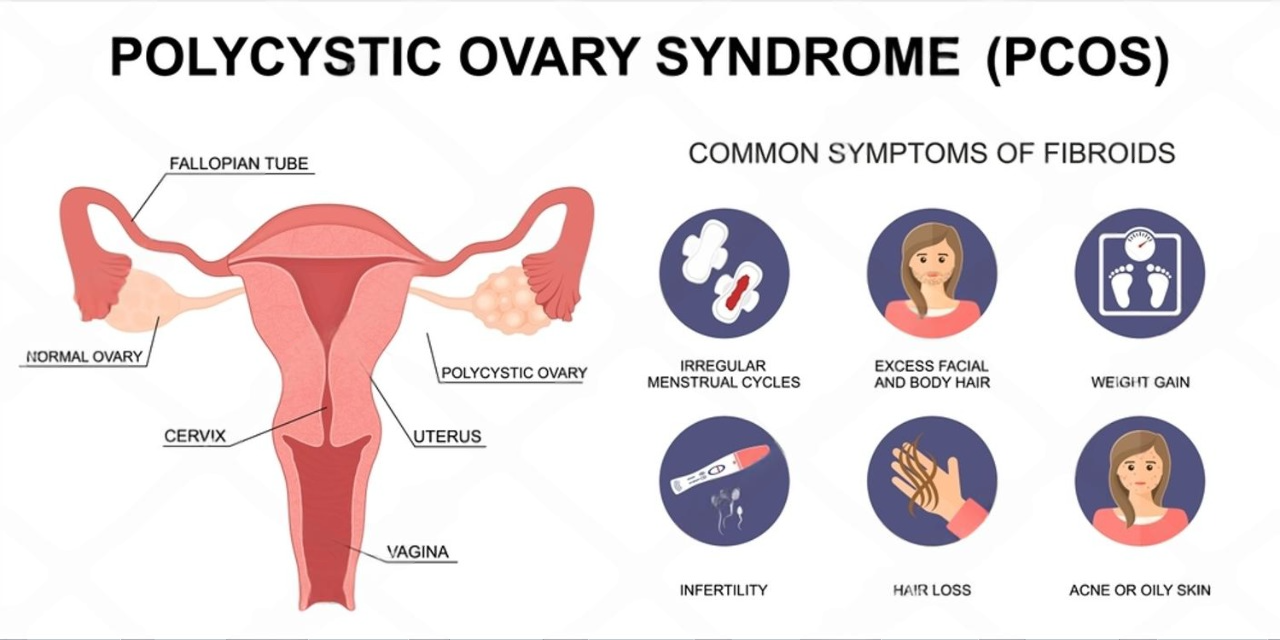
what is PCOS in teenagers?
PCOS is a hormonal disorder that can cause irregular periods, signs of excess male hormones (like acne or unwanted hair growth), and metabolic changes. In adolescents, diagnosing PCOS requires care because normal puberty can mimic many PCOS signs. That’s why Sparsh’s teen clinic follows the latest international guidance designed specifically for adolescents — focusing on menstrual irregularity plus clinical/biochemical hyperandrogenism, while excluding other causes. Adolescents with only one feature may be labelled “at risk” and monitored rather than immediately diagnosed.
Why teens are different: diagnosis and timing
Puberty is a time of biological change. Irregular cycles, acne, and some hair growth are often normal in the first few years after menarche (first period). International recommendations therefore caution against quick labelling of PCOS in girls soon after menarche and advise clinicians to use adolescent-specific diagnostic criteria and careful follow-up. When symptoms are severe (very infrequent periods, very heavy bleeding, rapidly worsening acne/hirsutism, or signs of another disorder), immediate evaluation is warranted.
At Sparsh Hospital we:
Ask about timing of menarche and cycle patterns.
Assess growth, weight, and family history (diabetes, metabolic issues).
Perform targeted blood tests to assess androgen levels and rule out other causes.
Consider ultrasound only when appropriate and interpret it cautiously in adolescents.
Common symptoms parents and teens notice
Teenagers with PCOS may experience one or more of the following:
Irregular or infrequent periods (cycles that are very long or absent).
Persistent acne or sudden worsening of acne despite normal treatments.
Increased hair growth on the face, chest, or belly (hirsutism).
Unexplained or rapid weight gain or difficulty losing weight.
Darkened skin patches (acanthosis nigricans) in neck/folded areas — a sign of insulin resistance.
Mood changes, anxiety, or low self-esteem related to appearance or menstrual problems.
If any of these cause distress, pain, or significant disruption to schooling or daily life, a medical review is recommended.
What causes PCOS in teenagers?
The exact cause is complex and involves genetics, hormones, and lifestyle. Key contributors include:
Elevated androgens (male-type hormones) in the body.
Insulin resistance, which can increase androgen production.
Family predisposition — PCOS often runs in families.
Lifestyle factors such as poor diet, low physical activity, high stress, and weight gain can worsen symptoms and metabolic risk.
Because insulin resistance is central for many adolescents with PCOS, addressing metabolic health is a priority.
How we evaluate a teen at Sparsh Hospital
Comprehensive history — menstrual pattern, acne/hair growth timeline, weight trends, family history, and psychosocial factors.
Physical exam — growth chart, BMI, blood pressure, skin exam (acanthosis nigricans), and hirsutism assessment.
Targeted investigations — hormonal blood tests (to check androgen levels and exclude other causes), glucose/insulin assessments as indicated, and selective imaging only when necessary.
Psychosocial screening — anxiety, depression, body image concerns and eating disorder screening when indicated.
Our adolescent specialists explain findings carefully to both teen and family, maintain confidentiality where appropriate, and involve the teen in decision-making.
First-line management: lifestyle is medicine
Lifestyle modification is the cornerstone of managing PCOS in adolescents. International guidelines emphasize that healthy eating, regular physical activity, improved sleep and stress management are first-line interventions — particularly for teens who are overweight or insulin-resistant. Lifestyle changes help restore more regular cycles, reduce androgen-related symptoms, improve insulin sensitivity, and protect long-term health.
Practical, teen-friendly strategies we teach:
Aim for regular physical activity (daily play, sports, yoga, brisk walking).
Encourage balanced meals emphasizing whole foods, vegetables, fibre and adequate protein; reduce high-sugar and highly processed foods.
Sleep hygiene: consistent sleep schedule and limiting late-night screen time.
Stress management: mindfulness, counselling, creative outlets and peer support.
Small, sustainable weight changes (5–10% of body weight) can produce major metabolic benefits.
Our multidisciplinary team (paediatricians, adolescent gynaecologists, dietitians, physiotherapists, and mental health specialists) creates realistic, non-stigmatizing plans tailored to each teen.
Medical treatments: when they’re needed
If lifestyle measures are insufficient or symptoms are severe, medical options may be recommended. Choices are individualized, with careful discussion of benefits and side effects:
Combined oral contraceptive pills (OCPs) — commonly used to regulate menstrual cycles and reduce acne/hirsutism. They’re often the first-line medication for menstrual irregularity and hyperandrogenic symptoms in adolescents.
Metformin — an insulin-sensitizing medication sometimes used when there’s clear insulin resistance, impaired glucose tolerance, or when weight and metabolic goals need medical support. Metformin can help metabolic markers and sometimes cycle regularity, but it’s not a universal option for all teens.
Topical and dermatologic treatments — for acne and hirsutism, we partner with dermatology for medications, procedures (like laser hair reduction when age-appropriate), and skin care regimens.
Anti-androgen drugs — used selectively and only with proper counselling and contraceptive cover; not first-line for most adolescents.
At Sparsh, prescribing decisions prioritize adolescent safety, growth considerations, fertility planning for the future, and minimal side effects. We follow the latest evidence and international adolescent-specific recommendations.
Mental health and body image: we don’t ignore this
Long-term health: prevention and monitoring
PCOS in adolescence is not only about immediate symptoms — it’s about long-term metabolic and reproductive health. Teens with PCOS have a higher lifetime risk of glucose intolerance, type 2 diabetes, cardiovascular risk factors, and infertility issues later in life. Early recognition, healthy habits, and appropriate medical care reduce these risks.
Follow-up at Sparsh Hospital typically includes:
Regular monitoring of weight, blood pressure and metabolic markers.
Screening for impaired glucose tolerance if risk factors are present.
Ongoing discussion about contraception, menstrual management, and future fertility planning.
Annual mental health review or sooner if needed.
We aim for proactive prevention and patient education to set teens up for healthy adulthood.
Practical advice for parents and caregivers
Listen and validate. Teens may feel embarrassed about symptoms. Reassurance and calm support matter.
Avoid premature labelling. Ask for a specialist review rather than relying solely on internet self-diagnosis or ultrasound reports. Overdiagnosis can cause anxiety and unnecessary treatment.
Support lifestyle changes together. Family meals, shared physical activity, and reducing household sugary snacks help.
Prioritise privacy and autonomy. Involving the teen in decisions builds trust and adherence.
Ask about mental health. If your teen shows mood shifts, social withdrawal, or eating disorder signs, seek help early.
A typical care pathway at Sparsh
Initial consultation — history, examination, baseline blood tests and psychosocial screening.
Personalised plan — lifestyle program, medical options if required, and referrals (derm, diet, mental health).
Follow-up visits — monitor symptoms, adjust treatment, repeat targeted tests as needed.
Transition planning — as teens approach adulthood we plan safe long-term care and fertility discussions.
